About one in five enrollees in Maine’s health insurance marketplace – 8,000 to 10,000 people – would have qualified for Medicaid had the state expanded the program for low-income Mainers under the Affordable Care Act, according to estimates based on numbers released by one of the state’s insurers.
The figures are the first glimpse at how the state’s decision not to expand its Medicaid program, MaineCare, has affected its health insurance marketplace, where people can buy subsidized insurance under the Affordable Care Act.
Republican Gov. Paul LePage, citing cost concerns, has vetoed several attempts by the Democratic-led Legislature to expand MaineCare and rebuffed efforts by moderate Republicans to forge a bipartisan compromise.
The first enrollment period ended March 31, with about 44,000 Mainers signing up for benefits.
A big question during the State House debate was whether the uninsured who would have been eligible for MaineCare under expansion would choose to remain without insurance or buy low-cost plans on the marketplace. About half of the 70,000 people who would have been covered were eligible to buy insurance on the marketplace with substantial payment assistance.
Republican legislators encouraged low-income people to sign up on the marketplace, even passing out pamphlets this spring to those rallying for MaineCare expansion at the State House.
Democrats viewed that suggestion as a political stunt or, at best, a half-measure that would leave 35,000 who didn’t qualify for subsidies without an affordable option.
Regardless, an estimated 8,000 to 10,000 people who would have qualified under the Medicaid expansion bought insurance on the marketplace in the first year it was available.
The U.S. Department of Health and Human Services has not released financial breakdowns of those buying insurance in the marketplace, and insurers do not receive income information from the federal government. But people with earnings at 100 percent to 150 percent of the federal poverty level – about $12,000 to $17,000 a year for an individual – are known to insurance companies because they are eligible for additional cost-sharing subsidies. MaineCare expansion would have covered adults earning as much as 138 percent of the poverty level, about $16,000.
Using figures provided by Maine Community Health Options, Mitchell Stein, a Cumberland-based health policy analyst, estimated that 8,000 to 10,000 people with marketplace plans would have qualified for MaineCare.
Stein’s estimate accounts for a more even distribution of enrollees throughout the income bracket. If more people earned closer to 150 percent of the federal poverty level, the estimate would be lower.
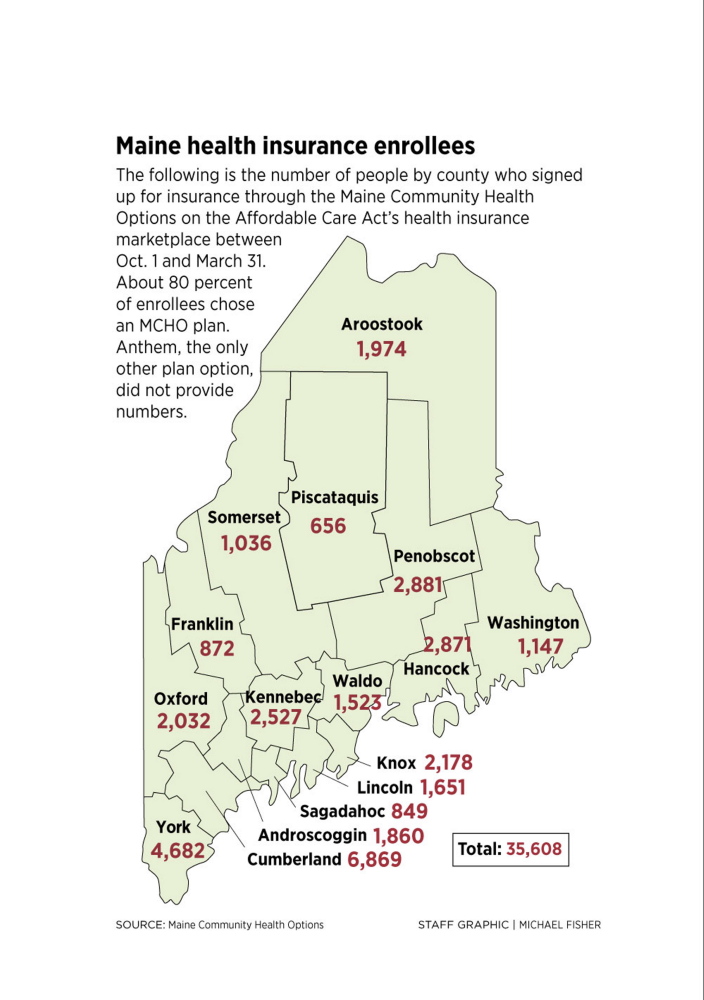
Maine Community Health Options has captured about 80 percent of Maine’s health insurance marketplace. Anthem Blue Cross Blue Shield, the only other Maine insurer that is selling plans through the marketplace, declined to provide figures.
Libby Cummings, who helped people sign up for health insurance at the Portland Community Health Center, said that for the most part, the low-income people she helped believed they could afford the premiums. They were willing to pay, rather than remain uninsured.
“People looked at it and said, ‘Of course I’m willing to pay for it.’ They felt like they were getting a really good deal,” Cummings said. “They were really proud to get insurance with a brand name.”
Although marketplace plans are not free, subsidies for the lowest-income residents drive down premium costs to about $10 to $15 per month. Additional cost-sharing subsidies available for residents with earnings at 100 percent to 150 percent of the federal poverty level further reduce the cost of insurance by helping to pay out-of-pocket costs such as deductibles or co-pays.
State Rep. Richard Malaby, R-Hancock, who serves on the Legislature’s Health and Human Services Committee, said he’s happy to hear that thousands took advantage of the health insurance marketplace and believes it will ultimately be better for the working poor than MaineCare expansion.
“If you have to pay a little bit of money, you value it more,” Malaby said. “They have some skin in the game.”
Malaby said the subsidies should also be made available to people earning less than 100 percent of the federal poverty level.
Subsidies are not available to the poorest residents because the Affordable Care Act mandated that all states expand Medicaid. However, a 2012 U.S. Supreme Court ruling allowed states to opt out. About half of the states have so far refused to expand Medicaid.
But Rep. Drew Gattine, D-Westbrook, another member of the Health and Human Services Committee, said the fact that some people are willing to pay for insurance is no reason to deny MaineCare expansion. More people would have benefited from expansion than the few thousand who gained insurance via the marketplace, he said.
The federal government would have paid 100 percent of the cost of MaineCare expansion for three years, and 90 percent in subsequent years, although Republicans have argued that there are many hidden costs.
Emily Brostek, associate director for the advocacy group Consumers for Affordable Health Care in Augusta, said low-income Mainers may not be able to pay for the modest premiums over time.
“If you’re living paycheck to paycheck, $15 a month can be a challenge,” Brostek said.
Kevin Lewis, president of Maine Community Health Options, said more than 90 percent of those choosing the insurer’s plans have paid their first month’s premiums.
But Cummings said the fact that Maine Medical Center and Mercy Hospital still offer free care to those who buy insurance on the marketplace is also an incentive.
For low-income Mainers who qualify, the hospitals would cover costs not paid by private insurance companies, Cummings said. She said if they hadn’t, it would have been a disincentive to buy marketplace insurance.
“It’s better for the hospitals because they get most of their costs reimbursed by private insurance, where the hospitals aren’t reimbursed at all for people who don’t have any insurance,” Cummings said.
Will Chapman, 23, of Greenwood would have qualified for MaineCare this year, but he said he probably would have declined the state coverage had it been available because he knew his income would likely increase.
Chapman, a student at the University of Maine at Augusta, earned about $12,000 per year working one part-time job, but he picked up another part-time job, which will double his earnings.
Chapman said he pays about $12 per month for marketplace coverage, although his premium will increase once he reports his new income.
Joe Lawlor can be contacted at 791-6376 or at:
jlawlor@pressherald.com
Twitter: @joelawlorph
Send questions/comments to the editors.



Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.