AUGUSTA — A year after opening a new hospital, officials report continued concern about a lack of beds but say the new design means fewer patient falls and a 20 percent reduction in the incidence of hospital-acquired infection.
“The good news is at least there’s nobody waiting in the emergency department for a bed,” said Chuck Hays, CEO of MaineGeneral Medical Center.
But he’s still smarting because the new building has 192 patient rooms, not the 226 rooms the hospital staff wanted. State regulators who signed off on the regional replacement hospital refused to approve the larger number.
“I think we’re still going to have some challenges with the size of the hospital,” Hays said, “but it won’t be as bad.” Complaints about capacity rose early when patients had to wait in the emergency room for a bed to become available, and some were given the option to go to other area hospitals.
He said he expects that challenge to increase, in the short term, particularly through the flu season.
The hospital had seen some good results after consolidating inpatient beds from the Thayer campus in Waterville and the former Augusta hospital on East Chestnut Street in the new 640,000-square-foot hospital at the north end of Augusta. The Thayer Center for Health underwent a $16 million renovation, but now it provides only outpatient treatment.
Hays said data collected from surveys showed higher levels of patient satisfaction, much lower instances of falls and a 20 percent lower incidence of hospital-acquired infection.
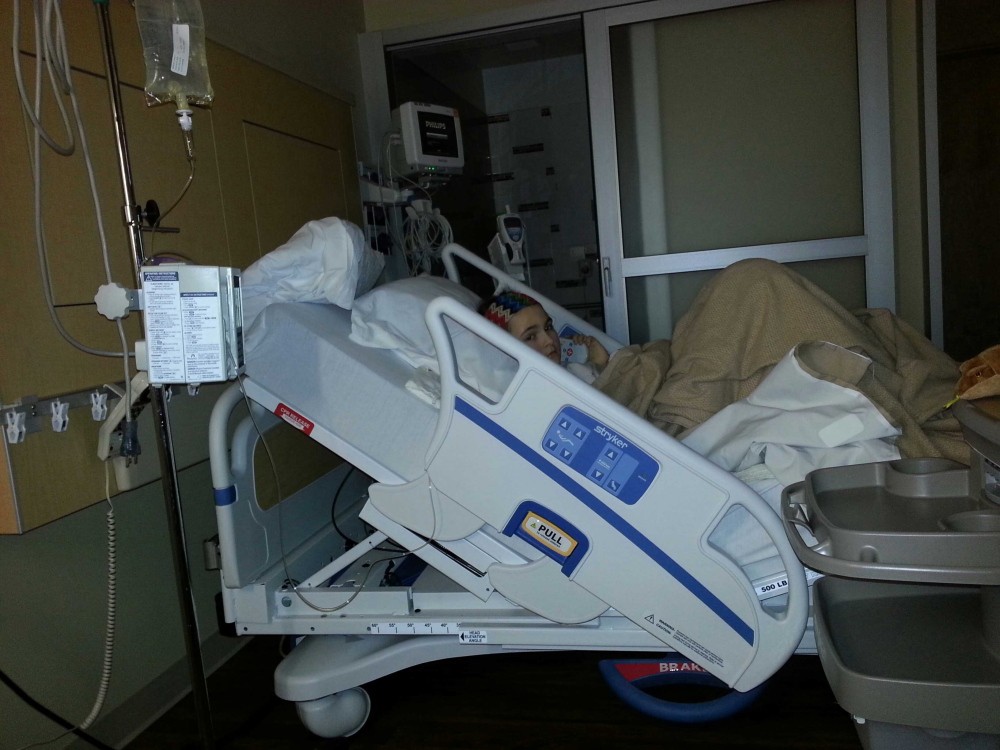
The hospital was designed to address some of those issues. All the 192 beds are in private rooms, handrails help steady a patient moving from the bed to the bathroom, and the average number of times a patient is relocated within the hospital generally is limited to moving from one level of care to another.
“All the indicators we’ve measured have improved,” Hays said, adding that it will take a year and a half for those to show up on some national databases. “One year later, we’ve gotten much more efficient.”
In fact, most outside agencies measuring hospital metrics have data relating to MaineGeneral’s performance in its previous hospital facilities. The most recent records end in June 2013, five months prior to the opening of the consolidated facility. Patients offered mixed reviews of the new hospital, with some offering praise peppered with a little criticism.
A LONG TIME COMING
Ray Veilleux, of Smithfield, said he encountered “wonderful doctors and wonderful treatment” for himself and for his 101-year-old father, who was admitted there after breaking his hip.
“The service and the people were unreal,” he said. “The problem I had was getting them to answer the darn telephone when it rings,” he said, specifically citing the emergency room and the cardiac care unit. “It’s the only complaint I have.”
Otherwise, he said, he and his late father received polite and professional treatment.
“I told my wife, ‘Bring me there; that’s where I want to go,'” Veilleux said.
The new hospital had been a long time coming and actually had been envisioned in at least one other location. MaineGeneral Health had operated two full-service hospitals within 21 miles of each other since the 1997 merger of Kennebec Valley Medical Center in Augusta and MidMaine Medical Center in Waterville. Portions of the former hospital campus on East Chestnut Street date to back to at least 1900.
In August 2005, the hospital bought more than 100 acres just off Old Belgrade Road as a place to build its $25.6 million Alfond Center for Cancer Care, an outpatient-only facility that opened in July 2007. With some adjacent land added, it became the natural location for the new regional hospital, and construction on that started in the summer of 2011.
The new hospital brought ancillary projects, including a $13 million road improvement project that connected the hospital to exit 113 of Interstate 95.
As soon as the new hospital opened, work began on Thayer, and that $16 million project was showcased for the public on Oct. 25.
The former hospital in Augusta and the former Seton campus in Waterville were bought by companies led by developer Kevin Mattson.
Jack and Anita Smart, formerly of Readfield and now at Granite Hill Estates in Hallowell, visited the hospital in late October with a $10,000 donation in gratitude for care Anita Smart received after suffering a stroke.
“We were happy to do it; it’s money well spent,” Jack Smart said. “Anita, my wife, was in the hospital for a week and then a week in therapy. All the nurses, doctors, all the rest of the staff, they all had smiles on their faces. It was very nice. They took care of her.”
On their way out, the couple hugged Vinnie Lord, a physical therapist who worked with Anita Smart.
“He’s a very positive guy and likable fellow,” Jack Smart said.
ER LAGS REPORTED
When the new hospital opened, the emergency room generated the most complaints, and some of those continue.
Mary Sprague, of South Gardiner, said her husband, Timothy L. Sprague, had a bad experience in the emergency room in May when he sought treatment for his sore foot.
“They don’t do nothing,” she said, adding that his problem was both diagnosed and treated at Central Maine Medical Center in Lewiston.
Dennis Horton, 69, of Gardiner, said he experienced both the good and the bad at the hospital. He had cancer surgery in September, which was delayed for hours, but the nurse kept him abreast of events and offered apologies for the unforeseen delay.
“A month prior to that, I had a chance to use the emergency room,” Horton said. “It was probably one of the worst experience I’ve had in my life.”
Horton said he went there seeking treatment for something that had gotten into his eye. He was triaged about 9 p.m. when he described the pain level as a 9 out of 10, and was told he was up next for care. Horton was particularly worried because a similar eye problem previously turned into an ulcer and effectively blinded him for three months.
After midnight, he asked how much longer it would take, and was told that cases were prioritized. He said he cut his wrist band off, saying he was going elsewhere for service, and received a laugh in response.
“I found out later everything that was done was not done right,” he said. “I ended up coming home and we treated it with some more medicine,” he said. In the future, he will head to Lewiston for emergencies unless he hears something has changed.
The hospital is responding to the concerns, and it has a patient advocate department to help patients with complaints.
“We are making ongoing improvements to our Emergency Department to reduce waiting times, including a (streamlining) project focus in the Emergency Department and will initiate a similar effort for inpatient flow,” hospital spokeswoman Joy Leach said via email on Friday.
Not all people reported problems in the emergency room.
Candace Sloma, of Augusta, was treated in the emergency room two days after the Nov. 9 opening.
“I was in and out of there in a matter of six hours,” she said. “I was amazed at the speed. They seemed to know what to do and where to go to get it. They were very efficient.”
Britt Holstrom-Salisbury, of Benton, and her family found great care for her daughter, Emma, then 11, a week after the hospital opened. Taken initially to the Emergency Department at the Thayer Center for Health, Emma was diagnosed with a kidney infection and sent by Delta Ambulance to the new hospital.
“When you have a child with autism doing something different and out of routine — such as being an inpatient at a hospital — it can be very anxiety-provoking for both the child and the caregivers. The doctors and nurses at both MGMC sites were open to hearing my suggestions on how to approach things with my daughter, and this made me feel as though she was in great hands,” Holmstrom-Salisbury said.
IMPROVED CARE FOR BABIES
Nikkia Veilleux, 30, of Waterville, and her husband, Timothy, had the first babies born at the hospital just after it opened.
“My experience was amazing from the very first time we walked through the doors,” Nikkia Veilleux said. “We were coming in as the patients were.” In fact, she had to wait a little for some hot water.
The twins, Hannah and Samuel, were delivered about six weeks before their due date.
A few hours earlier, and the babies would have been born in Portland; but the new hospital has a Level II Neonatal Intensive Care Unit, allowing it to handle such births and babies.
Veilleux said they were glad to be only 20 minutes from their home and son Isaiah Vear, now 8.
Over the past year, Veilleux and the twins visited the maternity ward so the staff could see how the twins were doing, and the hospital recently hosted an early birthday party for them.
“We’re part of the MaineGeneral family,” Veilleux said.
Another new mother, Brittany Adams, also enjoyed her experience there.
“My third son Gannon Noah was born at the new hospital,” she said in an email. “First of all it was great to have my (obstetrician) in the hospital. It made it easier to just go to labor and delivery when need be.”
Through Oct. 21, the hospital has delivered 1,036 babies.
BUDGET LOSS EXPECTED
Along with a number of physicians’ practices, housed in the Scott Bullock Medical Office Center, Hays said the new hospital also allows most administrators to be in the same building and much more readily available to meet, which is more efficient.
“We used to be in 10 different buildings,” he said.
Dollar figures, too, are on par with what the hospital anticipated.
Hays said the expectation was an initial two-year loss and a return to being 1 percent to 2 percent in the black by next year. The operating budget for the medical center itself is about $414 million for the current fiscal year, which began July 1, and includes the adjacent Alfond Center for Cancer Care, the Thayer Center for Health and the hospital’s physician practices. Hays also said the hospital anticipates a $5 million loss this year. Hays said a $16.4 million loss was anticipated last year, which ended up being $14.3 million.
The hospital’s fiscal year runs from July 1 through June 30. The hospital owned the former Seton campus of MaineGeneral Medical Center in Waterville until handing it over to the new owner, developer Kevin Mattson.
The hospital is a nonprofit organization and under the parent corporation MaineGeneral Health, which includes long-term care facilities and other health care operations.
It put out bonds to cover the vast majority of the $312 million in construction costs plus an additional $10 million to renovate Thayer and convert it to an outpatient facility with a 24-hour emergency department.
Annual repayment over as many as 30 years will average some $25.4 million, Hays said.
The hospital announced in June that it was cutting some 128 full-time positions, 16 of which were filled, as it prepared to enter a new budget year. It also trimmed discretionary accounts, such as travel. Those moves were necessary, Hays said at the time, because of lower Medicare reimbursement rates and anticipated decreases in patient volume as well as overstaffing that occurred when the hospitals were consolidated.
More recently, the hospital notified its 600 or so per diem staff members – nurses, maintenance, laboratory technician, house-keeping personnel, and others who are on call and who work less than full-time – that they would no longer receive a 10 percent differential beginning in January 2015.
“The majority of hospitals don’t pay a differential per diem,” Hays said. He said those workers have the ability to pick when and if they want to work.
Instead, Hays said, it will be adjusting its benefits plan to meet requirements of the federal Affordable Care Act.
MaineGeneral Medical Center employs about 2,400 people, of which about 1,700 full-time employees work at the hospital itself.
The hospital has had to make some adjustments for those workers as well, such as expanding the employee parking lot by 50 spaces in order to accommodate all the vehicles.
FEAR EASED BY CARE
The Rev. Lawrence “Bud” Merckens, 79, of Manchester, pastor of Riverside Congregational Church in Vassalboro, spent a week in the hospital with pneumonia last March.
“I couldn’t have gotten better services,” he said. “I was kind of worried about the hospital. I’m very suspicious of big things. I was completely wrong. It was very pleasant. Everyone went out of their way. I really felt quite relieved to be there.”
He said he enjoyed the meals; the fact that his wife, Hilda, could stay in the room with him; and even returning daily for two weeks for intravenous therapy.
“We’re very fortunate to have it in the community,” Merckens said.
Shelly Simpson, of Oakland, talked about care the hospital provided to her mother, Dolores Champine, 90, who had been living in Lakewood Longterm Care in Waterville for six months until she was hospitalized Oct. 7-24 in Augusta.
Simpson said she and Champine saw every aspect of the hospital from the emergency room, surgery, recovery, medical/surgical units and food service.
“I have nothing but wonderful things to say about the care she received in her final days,” Simpson said. “I was there every day, all day, and some nights as well.”
Simpson described her mother, a former director of nurses at Waterville Osteopathic Hospital (now Inland Hospital) as a “spitfire just till the very end.”
When three nurses took care of her at MaineGeneral, she told her daughter, “This is like private-duty care when I was a nurse.”
“If that comment didn’t speak volumes, I don’t know what does,” Simpson said. “Being there and being an advocate for my mom, the compassion was amazing. You felt you were the only person in that hospital.”
Betty Adams — 621-5631
Twitter: @betadams
Send questions/comments to the editors.








Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.