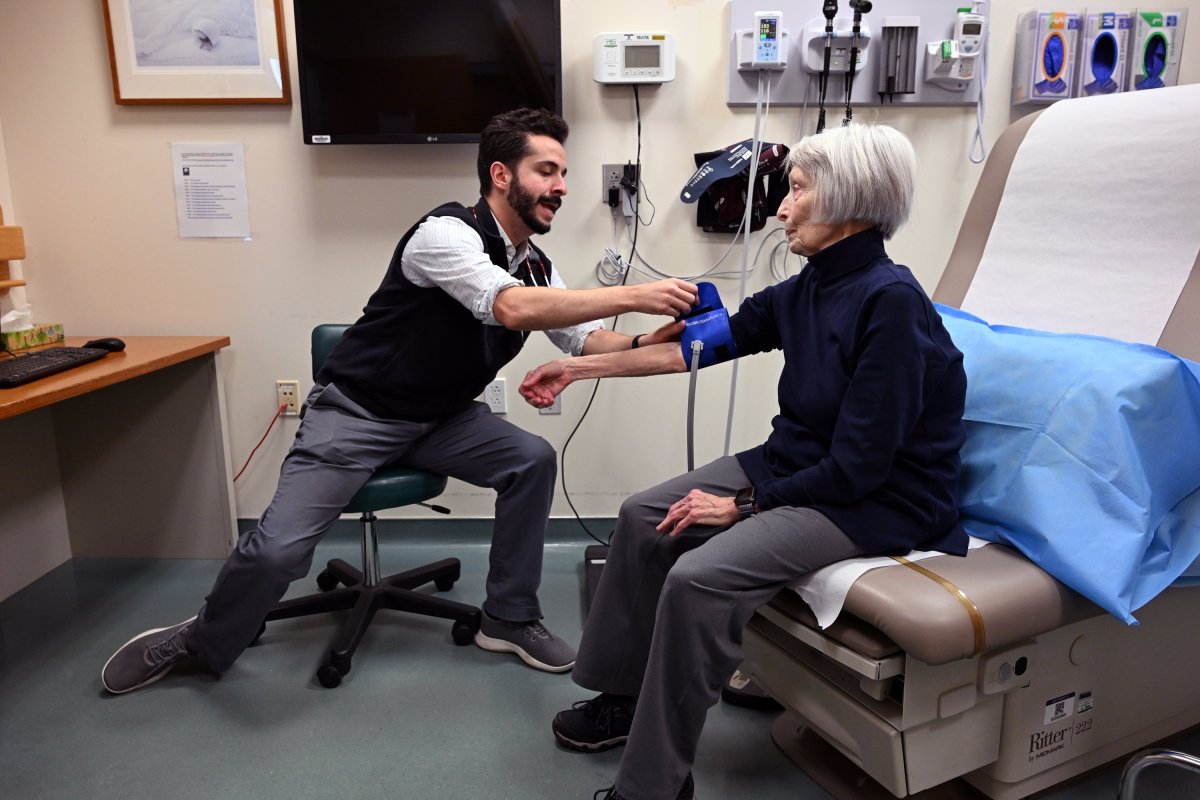
Dr. Zach Duperry listened while his patient recounted her recent trip to England. It was a memorable vacation — but not in the way she wanted it to be.
“I went to Stonehenge, had some fish and chips, and then I was sick the entire time after that,” said Betsy Beecher, 81, laughing during her January appointment. She spent three days at Maine Medical Center after she returned, being treated for pneumonia.
“That’s some bad luck, my friend,” said Duperry, who is in the second year of his residency at MaineHealth Primary Care in Portland’s Munjoy Hill neighborhood.
Duperry, a 30-year-old Portland native, said he knew he wanted to stay in Maine after graduating in 2024 but, like many doctors, had barriers to overcome in order to work in the state.
Experts say Maine has been grappling with a shortage of primary care physicians and increasing the workforce is hampered by several issues, including the state’s lack of residency programs, the high cost of medical school coupled with lower pay, health systems in financial jeopardy and doctors preparing for retirement.
Across the U.S., the Association of American Medical Colleges projects the shortfall of primary care physicians could reach between 20,200 and 40,400 by 2036. The need in Maine is high, experts say, because of the increasing and aging population.
“The state needs more residencies, that is the bottleneck,” said Dr. Linda Chaudron, vice president of medical education at MaineHealth. “We can graduate as many as we want, but if there’s not enough residencies, we are going to have a harder time getting people to stay here.”
Maine’s health care systems, universities and some state lawmakers have sought solutions to ease the shortage, including increasing the number of residency programs, providing financial incentives to practice in rural areas and boosting the money for medical school scholarships.
Across the state, there are about 70 primary care residency slots, said Dr. Jane Carreiro, vice president of health affairs and dean of the College of Osteopathic Medicine at the University of New England.
Duperry, who graduated from the Maine Track program, which is a partnership between Tufts University School of Medicine and MaineHealth, said he applied for 10 residencies, most outside of the state.
Portland was his top choice.
“I’m from here, my family is here,” Duperry said. “It’s a community I really feel invested in long-term.”
Dr. Debra Rothenberg, the attending physician at the Portland practice, is Duperry’s mentor and someone he has known since he played soccer on the Deering High School team with her son.
“He is an example of what Maine needs,” Rothenberg said. “He’s dedicated to being here and practicing medicine in Maine.”
INCREASING THE WORKFORCE
A residency is typically a three-year training after medical school where doctors practice with an attending physician. In a recent graduating class, about 90 UNE medical students applied for and were selected into primary care residencies, but only 25 were based in Maine, Carreiro said.
Chaudron pointed to research that shows about 55% of primary care physicians practice near where they did their residency, and doctors are even more likely to stay in-state if they completed medical school there, further strengthening their ties.
Dr. Gavin Ducker, MaineHealth’s senior medical director for administrative and clinical affairs, said “we are not going to be able to recruit our way out of this,” but that the hospital system has a team working to recruit medical professionals to Maine, with a focus on primary care doctors who have connections to the state.
“If they trained or lived here or went to school here, we are interested in them,” Ducker said.
Carreiro said launching a residency means a practice has to have enough capacity to take on a doctor who needs to be mentored and trained for three years, at a time when health systems are struggling financially and dealing with workforce shortages.
Maine has taken some strides, such as creating a collaborative between the state’s major health systems in 2022 that helped launch four rural residencies and made other medical education investments.
UNE and MaineHealth are also looking at ways to increase the award for the Doctors for Maine’s Future Scholarship, which helps pay for the cost of medical school.
A bill proposed last year that would have used $1.9 million in state tax dollars to boost rural medical education, including adding clinical rotations at primary care sites for third and fourth-year medical students, stalled in the Legislature. That bill was carried over to the current session.
Since 2009, MaineHealth has partnered with Tufts University for the MaineTrack program, which has medical students doing much of their learning in the state.
A study done in 2025 for the University of Maine and the Maine Legislature said the state is projected to be short 120 primary care doctors by 2030. That estimate is based on a report by the Robert Graham Center, a national think tank, using data from 2010.
According to the U.S. Bureau of Labor Statistics, there were 630 family medicine doctors in Maine in 2024, down from 710 in 2019. Those numbers do not include all primary care physicians, who could be categorized in pediatrics or other areas, like internal medicine.
Improving access to primary care also means increasing the number of physician assistants and nurse practitioners in Maine, said John Vitale, dean of the Westbrook College of Health Professions at UNE.
According to the Bureau of Labor Statistics, the number of nurse practitioners and physician assistants in Maine increased from 2019 to 2024, but how many work in primary care is not specified.
“It used to be the doctor did everything, everything was ‘doctor-centric.’ That’s not sustainable,” Ducker said. “We have to have a care team that includes pharmacists, dietitians, physical therapists, social workers, and NPs and PAs. They all perform very important roles.”
HIGH COSTS
Compounding the problem are the financial concerns within the state’s hospital systems, the health care workforce shortage and a large number of doctors reaching retirement age. About 32% of primary care doctors in the state are age 60 or older, according to a 2024 report by the National Center for the Analysis of Healthcare Data.
But a top issue, experts say, is the high cost of medical school.
Duperry said he has had to navigate how to afford the $400,000 medical school price tag. The Doctors for Maine’s Future program took care of about $100,000, but the rest he had to take out in student loans.
That’s a lot of money to pay back on an average $240,000 per year salary — a disincentive compared to what he could have been making as a specialist, potentially earning $500,000 or more.
Duperry said the idea of doing what he can to improve Portland’s health was more appealing.
“I like having more of a focus on treating entire families and communities, learning why people get sick, and what can be done to make them healthy,” he said.
Not everyone is making that same calculation.
“Unfortunately when students are graduating with $250,000 or more in student loan debt, when you look at what primary care pays, it’s not the most attractive financially, even though it’s one of the most fulfilling things you can do in your life,” Carreiro said.
GRADUATING MORE DOCTORS
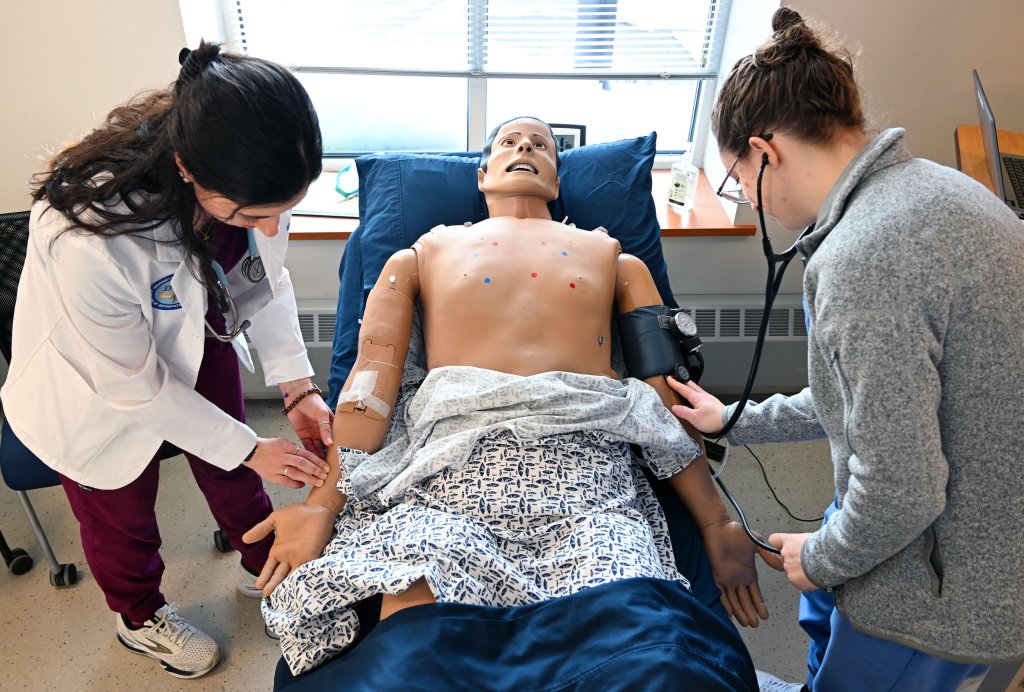
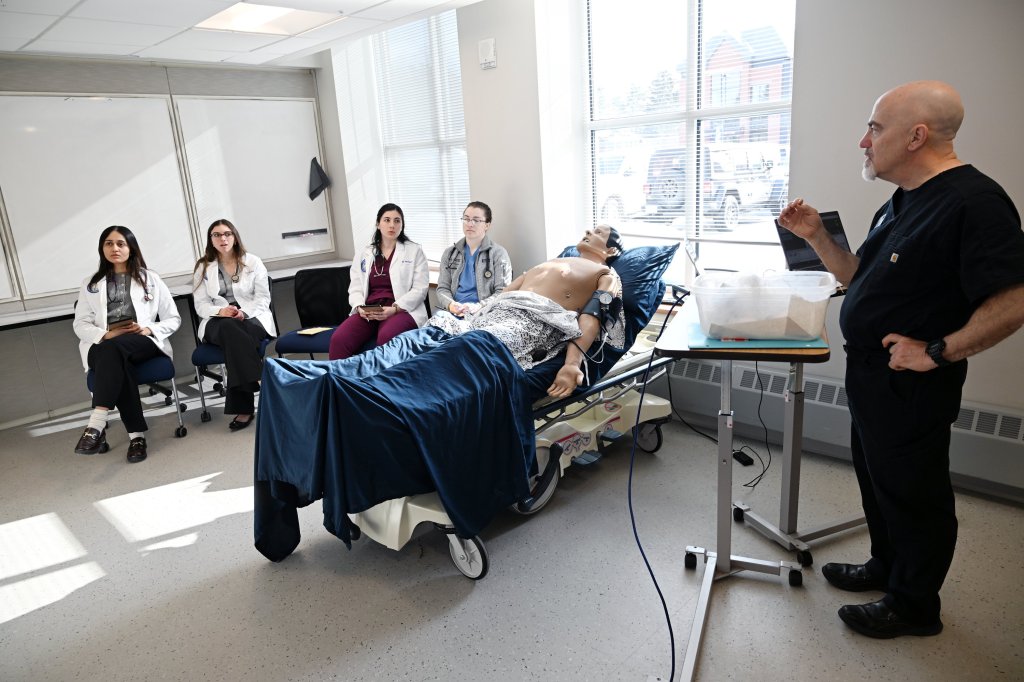
During a recent class at UNE’s Portland campus, first-year medical student Emily Harris took a test using a roboticized mannequin, taking its pulse, respiratory rate and blood pressure. The mannequin’s chest moved up and down, simulating breathing.
Harris, who grew up in rural Yampa, Colorado, said she’s interested in going into primary care partly because she grew up in an area where the closest hospital was a 45-minute drive away.
“I have first-hand experience, seeing that shortage of accessible health care myself,” Harris said.
After UNE shifted its medical school from its Biddeford campus to a new 110,000 square-foot building in Portland last year, it increased its graduating class from 165 to 200. The first class with 200 students will graduate in 2029.
The MaineTrack program — the partnership between MaineHealth and Tufts — graduates 40 students per year.
A 2025 study found that while the state will need more primary care doctors in coming years, it isn’t currently financially feasible to build a new medical school at the University of Maine. According to the report, it would cost $250 million to start up and $22.5 million annually to keep going.
Many medical school graduates, experts say, don’t go into primary care. Harris, though, said she’s interested in rural health care and would consider staying in Maine after she graduates.
“You can be of service to so many people in underserved areas,” Harris said. “And from a medical perspective, in primary care there’s a lot of variety. You’re going to be seeing new things that challenge you, and you’re going to need a lot of problem solving and critical thinking.”

As Duperry consulted with Beecher — his patient during an appointment in late January — about her medications, he took her blood pressure and examined her vital signs. She checked out well.
“I’m back to doing all my normal things, yoga and swimming,” Beecher told him.
She wasn’t excited about taking pills he prescribed her to help with iron deficiency, but took Duperry’s advice.
“I’m glad he’s here. He’s very personable with his patients,” Beecher said. “He listens well and he’s wicked smart.”
Editor’s note: This story was updated on Feb. 27 to correct what year of residency Dr. Zach Duperry is in and when he graduated.

We invite you to add your comments. We encourage a thoughtful exchange of ideas and information on this website. By joining the conversation, you are agreeing to our commenting policy and terms of use. More information is found on our FAQs. You can update your screen name on the member's center.
Comments are managed by our staff during regular business hours Monday through Friday as well as limited hours on Saturday and Sunday. Comments held for moderation outside of those hours may take longer to approve.
Join the Conversation
Please sign into your CentralMaine.com account to participate in conversations below. If you do not have an account, you can register or subscribe. Questions? Please see our FAQs.