RICHMOND — Edward “Chuck” Clark, a 73-year-old veteran of the U.S. Air Force and a retired poultry farmer, has trouble living independently. He injured his back a few years ago and more recently fractured his hip in a fall, requiring a partial hip replacement. He now uses a walker and does physical therapy exercises every day.
But while Clark, a Starks native who served from 1962 to 1966, has lived in a nursing home in the past, he much prefers the home where he now stays.
“The food’s a lot better, and the environment is a lot better,” he said. “I can get out and go places here, but (at the nursing home) we didn’t.”
That home belongs to — and the blueberry pie and bacon-wrapped scallops are prepared by — Sherolyn Dyer.
Dyer, a Richmond retiree who once worked as an administrator for a residential care organization, began looking after veterans seven years ago. She has done so through a program developed by the U.S. Department of Veterans Affairs and administered at the state level by the VA Maine Healthcare System at Togus.
With VA funding, Dyer and her late husband built ramps and made other physical improvements to allow those with disabilities to stay there. They also committed to serving as caretakers for the veterans: preparing their meals, washing clothes, taking them on excursions outside the home, passing a variety of inspections, arranging for hospice care workers to come at the appropriate time.
Since then, five veterans have stayed with Dyer, who is 65. The veterans pay her directly for the service, but looking after them hasn’t felt like work, said Dyer, whose husband, Ronald, was in the Air National Guard and whose father and brother both served in overseas wars.
“I view it as my lifestyle,” she said. “When people have fought and done hard things for us, I think they deserve the best care.”
The medical foster home program, as it’s called, is just one way the VA — like the U.S. health care system as a whole — has been responding to the needs of an aging population.
Though the total number of patients enrolled in the Maine system is projected to decline over the next two decades, from 54,016 in 2015 to 48,460 in 2035, administrators expect the proportion of Togus enrollees who are older than 65 to hover around 55 percent.
“The challenge of the last 10 years has been the continued needs of the aging portion of the veterans population and a whole new set of needs for the younger group,” said Ryan Lilly, director of the Maine system. “Still the greater volume need is older vets, and also for the younger group as they age.”
One of the physical expansions that is planned for the main Togus campus in Chelsea is a new, long-term care facility that will be built over the next five or 10 years, Lilly said.
The system has outpatient clinics located around the state and a host of other programs that are meant to let veterans age in place.
One of them is a primary care program that sends physicians, nurses, dietitians, social workers and occupational therapists to check on veterans at their homes. Togus has also implemented a telehealth program that provides monitoring devices to patients who are at risk of conditions like congestive heart failure, allowing the patients to perform daily monitoring of their blood pressure, weight and pulse, the results of which are sent to a panel of Togus nurses.
If any of those levels seem unhealthy, Lilly said, the nurses can speak with a designated, full-time doctor and recommend changes in the amount of medication a patient should take. The program has led to an 80 percent reduction in the number of patients who are readmitted to the hospital, translating to fewer costs for Togus as a whole, Lilly said.
Togus administrators also point to the medical foster home program as a boon for the federally funded system.
Though a quarter of veterans in the program qualify for nursing home care that is fully funded by the VA, they choose to spend between $1,500 and $3,000 of their own funds to stay with a family, according to an information sheet updated by the VA in August.
Those fees go directly to caregivers like Dyer, said Morgan Delattre, who coordinates Maine’s medical foster home program. For each patient in the program, meanwhile, the VA pays about $10 per day in administrative costs.
Since starting in Maine in 2010, the program has served 94 veterans, Delattre said. Thirteen foster homes, spread between central and southern Maine, are now serving 16 veterans. Nationwide, there about 1,000 veterans enrolled in foster care programs.
Clark, the Air Force veteran, has stayed in two foster homes. He first stayed at one in Mexico, but for reasons that he declined to provide, that situation did not work out.
But Dyer’s home, he said, is “very worth” the monthly expense. He reads as many free mystery novels as he can find on his Kindle device. He has two grown daughters who live elsewhere in the state and visit him. Beyond the meals and the comfortable living space, he also appreciates the chance to go on excursions with Clark for shopping and fun.
“We’re a very active house,” said Dyer during an interview in her kitchen. “It helps to keep them feeling alive and worthwhile.”
“That’s very true,” Clark agreed.
Charles Eichacker — 621-5642
Twitter: @ceichacker
Copy the Story LinkSend questions/comments to the editors.


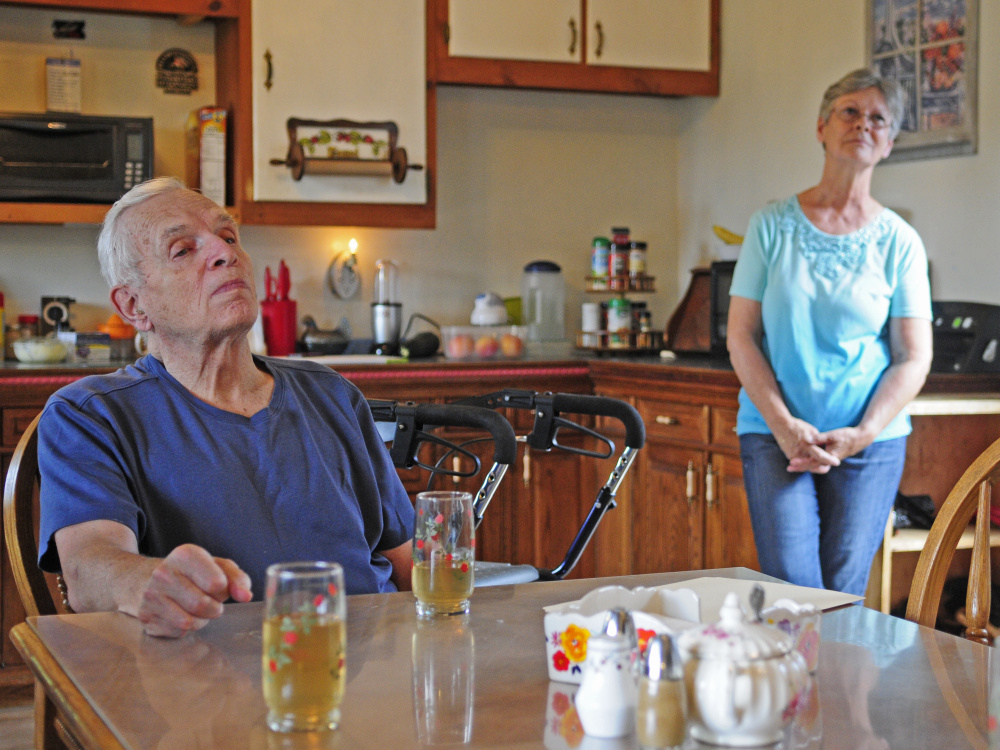




Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.