Medicaid expansion would substantially jump-start access to opioid addiction treatment for low-income Mainers at a time when the state is struggling to reduce drug overdoses and contain the opioid epidemic.
But whether a positive vote on the Nov. 7 ballot question would translate into reduced overdose deaths or an overall alleviation of the opioid crisis is difficult to predict, health experts say.
“Medicaid expansion gives people an on-ramp for medication-assisted treatment, which is the gold standard for opioid treatment,” said Dr. Richard Frank, a Harvard Medical School professor of health economics and former Obama administration official who helped implement the Affordable Care Act.
Frank said many factors contribute to the opioid crisis, so it’s not certain yet whether states that have expanded Medicaid have a head start on mitigating the epidemic. Part of the problem, he said, is that the opioid problem was generally worse in Medicaid expansion states before the Affordable Care Act went into effect in 2013.
“We haven’t been able to sort that out yet,” Frank said. “This crisis has been 20 years in the making. This is not something you can turn around quickly.”
If voters approve the referendum, Maine would join 31 other states that have expanded Medicaid. Maine Gov. Paul LePage, a steadfast opponent of expansion, has vetoed five attempts by the Legislature to approve expansion, which is a cornerstone of the ACA but voluntary for states.
Proponents of expansion view access to opioid treatment as one of the tangible benefits of expansion. Opponents say Medicaid expansion would bust the state’s budget, pointing to a previous expansion that was followed by repeated budget deficits.
About 70,000 Mainers would be eligible for benefits if voters approve the ballot question. Currently, about 265,000 Mainers have Medicaid coverage.
It’s difficult to say how many of those 70,000 need treatment for opioid addiction. A study of four states by the Government Accountability Office estimated that 13 percent to 35 percent of the Medicaid expansion population in the states of New York, West Virginia, Iowa and Washington abused or were dependent on opioids.
If 15 percent to 35 percent of the expansion population in Maine had an opioid problem, that would translate to 10,000 to 25,000 people who could seek medication-assisted treatment under Medicaid.
Medication-assisted treatment pairs counseling with drugs such as Suboxone, methadone and Vivitrol, which reduce the cravings associated with addiction. Research shows that this is the most effective treatment method to prevent people from relapsing into opioid use. In Maine, 376 people died of a drug overdose in 2016 – a record high – and 2017 is shaping up to be similar, with 185 deaths through June 30.
WITHOUT TREATMENT, A ‘HAMSTER WHEEL’
Access to medication-assisted treatment in Maine is difficult to come by. In Scarborough, the police department’s Operation Hope sends many people out of state for treatment because of the lack of options in Maine.
Those in the treatment community say that without insurance, addicts find themselves on a “hamster wheel,” in which they overdose and, if they survive, go to a hospital emergency room before being sent home. The cycle then repeats, and paramedics and hospitals often see the same people struggling with addiction and no access to treatment.
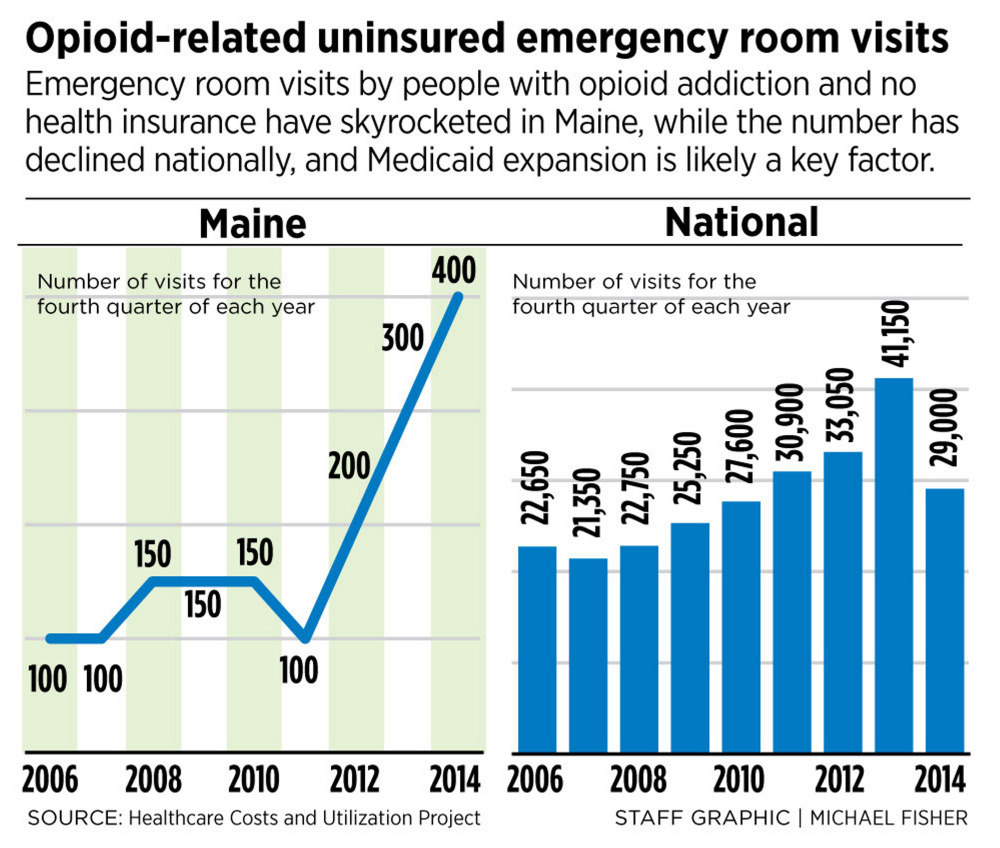
This cycle is straining the resources of hospitals – especially rural hospitals that are already struggling financially, according to federal data. Nationally, there were about 140,000 opioid-related hospital visits in the fourth quarter of 2014, but visits by uninsured patients declined in that time period from 41,150 in 2013 to 29,000 as most states expanded Medicaid.
In Maine, opioid-related visits totaled 1,100 in the fourth quarter of 2014, but those without insurance grew from 300 in 2013 to 400 in 2014, according to the U.S. Department of Health and Human Services.
Jeffrey Austin, vice president of government affairs for the Maine Hospital Association, said hospitals’ emergency departments have an “uncompensated care burden” when the uninsured overdose.
“Coverage is a good thing for all medical conditions, but there is clearly a need for more coverage for those in need of help with substance use disorders, particularly those that are opioid-related,” Austin said. The hospital association supports Medicaid expansion.
The uninsured dynamic is pronounced at Milestone Recovery, which operates a detox center in Portland.
Bob Fowler, Milestone’s executive director, said the center used to get patients with Medicaid, but now more patients are uninsured, as their addictions make them unstable and they lose their jobs. The LePage administration tightened eligibility for Medicaid so that childless adults would not qualify, and made it more difficult for parents to qualify for Medicaid.
These are “the very same people who are coming to Milestone, and they don’t have Medicaid anymore,” Fowler said.
‘MAINECARE WAS A LIFESAVER FOR ME’
The agency had a $3.7 million budget in 2011, before the Medicaid cutbacks, and that has dwindled to $3.1 million in 2017, Fowler said. Medicaid funding declined from $1.9 million to $586,000 during that time.
“It has had a strangling effect,” Fowler said, as Milestone has had to cut staffing. The program’s Old Orchard Beach residential recovery program often has empty beds because not enough people have Medicaid, and the program can’t afford to give too many people free care.
Fowler said people discharged from detox would have more options with Medicaid, including residential and outpatient treatment programs, instead of going home and falling into the trap of using again.
Kirk Carlsen, a housing navigator at Milestone, said he was one of the lucky ones. His heroin addiction was at its worst when he checked in to Milestone’s detox program on New Year’s Day 2013. As a childless adult, he had Medicaid, but it was set to be cut off by the LePage administration in 2014.
Carlsen had a year to straighten his life out, and having Medicaid – called MaineCare in the state – gave him access to counseling and Suboxone. After a year, he got a part-time job working for Milestone and was able to obtain insurance through the Affordable Care Act, and now he has a full-time job and employer-based insurance.
“MaineCare was a lifesaver for me,” said Carlson, 53. “I would be dead or in jail right now.”
Many in the expansion population can get insurance now through the Affordable Care Act, a point emphasized by state Rep. Karen Vachon, R-Scarborough, an expansion opponent. The Kaiser Family Foundation has estimated that about 21,000 Mainers who earn between 100 and 150 percent of the federal poverty limit have ACA insurance. If Maine approves expansion, those earning between 0 and 138 percent of the poverty limit would go on Medicaid.
Vachon said it would be better for that group to stay on private insurance through the ACA.
“People would rather have private insurance and have a job, rather than be on welfare,” she said.
THE CASE FOR PRIVATE INSURANCE
Vachon maintains that a bill she has proposed to help the uninsured would be a better solution than Medicaid. The bill, which she said stalled out this year in the Legislature but will be reconsidered in the next session, would devote more than $6 million a year to expand opioid treatment to help the uninsured.
She said the idea would be to give medication-assisted treatment to people struggling with addiction and then get them working as quickly as possible, so they would then qualify for ACA insurance. Those who are unemployed but find jobs qualify for “special enrollment” and can fairly quickly get ACA insurance, Vachon said.
“With private insurance, people would have access to a stronger provider network, the insurance has better reimbursement rates for doctors and better access to care,” she said. “We can move them off of welfare, get them jobs and help more people.”
But Dr. Lisa Letourneau, a public health expert who previously served on the Maine Opioid Collaborative, said that Medicaid expansion is by far the best option to provide access to treatment. The federal government would pay for more than 90 percent of the cost of expansion, and Letourneau said the state would tap into that money for treatment.
The Legislature’s nonpartisan Office of Fiscal and Program Review estimated the state would spend $93 million in state tax dollars on expansion through 2019, but receive nearly $1.2 billion in federal funds.
“There is no magical money for treatment without doing expansion,” Letourneau said. “Providing access to treatment for people with addiction is critically important both to the state as a whole and to those individuals and families. They have real and significant barriers to care. These are evidence-based treatments that we know will help them with their recovery.”
Joe Lawlor can be contacted at 791-6376 or at:
Twitter: joelawlorph

Comments are no longer available on this story